Global Allocation of the COVID-19 Vaccine and Its Ethical Implications
Nicole Boardman ’22 is a junior majoring in biology and a 2020-21 health care ethics intern at the Markkula Center for Applied Ethics. Views are her own.
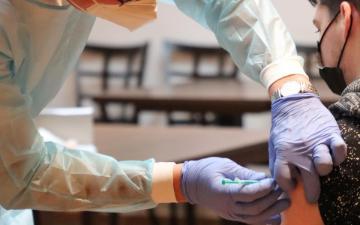
On December 14th, the first doses of the COVID-19 vaccine administered in the United States were given to healthcare workers, sparking a sense of hope across the country for an end to the coronavirus pandemic. For the United States, Canada, the United Kingdom, and other developed countries, the long-awaited end was very much in sight. This was not the case for citizens of the developing world. According to a study by the British Medical Journal (BMJ), over half of the reserved doses of available vaccines have been purchased by the world’s wealthiest countries despite these countries only making up 14% of the world’s population. The study predicts that a quarter of the global population will not have access to a vaccine until 2022, and we likely won’t see a fully COVID-vaccinated world until 2023 or 2024. Exacerbating the shortage of available vaccines in lower-income nations is the issue of hoarding by higher-income nations. Canada, for example, has purchased enough of the vaccine for each of its citizens to receive 9 doses. This leaves low-income countries at the mercy of ones that have stockpiled, as they are now relying on donations or “leftovers” to contribute to their supply of doses. This begs the question: is this the best we can do for the world? How can we apply ethical principles to the allocation of the COVID-19 vaccine to guide us towards a more equal and fair approach?
First, wealthy countries must acknowledge the social, ethical, and economic responsibilities they have to ensure that vaccinations are also available for poorer countries. Developing countries are the most vulnerable to the effects of the pandemic due to lack of medical capacity and economic infrastructure to respond and recover. Citizens of wealthy countries also often have luxuries that many around the world do not, such as a home in which to self-isolate and technology in order to work from home. These luxuries provide the means by which citizens of wealthier countries can mitigate the spread of the virus. For citizens of developing countries where homelessness and poverty are widespread, immunization is the only viable option to protect themselves from the virus and maintain their livelihoods.
A universally accepted goal of medicine is to impart the most amount of good onto the most amount of people, and to limit suffering wherever possible. It would then make the most sense ethically to grant priority to groups of people who are the most vulnerable and have the greatest risk of suffering because of the virus. As a society, we should prioritize the needs of the disadvantaged, especially in the context of global health. Countries with the capital and infrastructure already in place have a moral responsibility to provide pandemic relief to those countries that lack similar resources. Even from an economic standpoint, it makes more sense for developed countries to take on the responsibility of creating vaccine access for developing countries. Because of our inextricably connected economies and the globalized nature of our world, no country is exempt from pandemic consequences until all countries are protected. In fact, about 70% of the world population would need to be vaccinated in order to control the pandemic and establish immunity. Studies have shown that wealthier countries will actually suffer more financially by not helping poorer countries recover from the pandemic sooner. The SARS-CoV-2 virus does not know borders, skin color, or socioeconomic status. To treat this as an isolated issue amongst individual countries and expect a quick, minimally damaging recovery, would be naive.
Alongside wealthy countries, pharmaceutical companies have an important role to play in promoting just distribution of the vaccine. These companies have a moral obligation to ensure that their products are distributed in line with need and not rely solely on political or economic motives. AstraZeneca notably pledged to sell their vaccine on a “not-for-profit” basis in developing countries, showing the company’s active efforts in trying to close the accessibility gap. Still, one company cannot solve an issue that affects more than half the globe. AstraZeneca’s contribution will only provide enough vaccines for 18% of the world population at most.
Safety and efficacy must also be accounted for in equitable distribution. Pfizer/Biontech and Moderna are arguably the most safe and effective vaccines on the market right now, both showing well above 90% effectiveness with the data to back it. And yet, the People’s Vaccine Alliance reports that the entirety of Moderna’s supply and 90% of Pfizer/Biontech’s have been secured by wealthy developed nations. Meanwhile, China has stepped forward to provide a vaccine for developing countries in Africa, the Middle East, and SouthEast Asia to fill the role left vacated by the United States as a global health leader. However, the safety and efficacy of the Chinese-developed vaccine has been questioned by many due to the lack of transparency in reporting their scientific data. As a result, many see this as a soft-power move by China, suspecting that they are using the vaccine crisis to reach diplomatic ends. What does this say about the value that the pharmaceutical industry places on money and political agendas versus the value it places on equal and accessible treatment? Vulnerable countries should not be treated as pawns in diplomatic schemes, nor should they be left out of deals for vaccine options. Everyone has a right to safe and effective medicine, so pharmaceutical companies should uphold their ethical obligation to prevent the COVID-19 vaccine from entering a capitalistic hierarchy where the rich get priority access to the best treatment while the poor get whatever is left.
Not only does “vaccine nationalism” have direct effects on health and economic outcomes of individual countries, it has broader implications on society’s view of human rights in the context of medicine. How can we as a just society turn a blind eye to hoarding vaccine doses and neglecting disadvantaged peoples? The current actions of world leaders and Big Pharma demonstrate to the world how little they value healthcare as a basic human right, as well as setting a precedent for addressing future large-scale disasters. Will our moral obligations always stop at our own borders? The lack of collaboration among and within nations has resulted in prolonged consequences that are disproportionately affecting vulnerable populations. Not only is this “every-country-for-themselves” mentality morally wrong, it is counterproductive to the universal goal of pandemic recovery. Simply accepting health inequity as an unavoidable obstacle in order to justify the prioritization of wealthy countries in this pandemic opens the door to the acceptance of any moral wrong that is difficult to overcome as a way to perpetuate practices that benefit the privileged few.
So what should we be doing to ensure equitable global vaccine distribution? One initiative already in place to address vaccine disparities is COVAX (COVD-19 Vaccines Global Access Facility). This effort, led by the World Health Organization (WHO), allows countries to donate money towards an array of vaccine candidates to be purchased and delivered to developing nations. The issue with COVAX is that the initial phase administers doses to each country in proportion to their respective populations, which wrongly assumes that health and economic impacts of the pandemic are equally distributed. The Fair Priority Model, authored by a group of bioethicists, proposes that instead of allocating doses in proportion to population, we should allocate doses in line with need. The model outlines 3 phases in a triage-like fashion, starting from allocating resources to the most severely affected where the most suffering can be prevented, and ending with transmission reduction and restoring society to a sense of normalcy.
The Fair Priority Model draws on the values of maximizing good and reducing harm while limiting discrimination based on race, religion, and other factors that are not morally relevant to vaccine distribution. It commendably takes into account the disproportionate effects of the pandemic in different countries in order to maximize the collective good. The model’s authors call on world leaders and pharmaceutical companies to work together through initiatives like COVAX to address the pandemic on the global stage. Analyzing global vaccine allocation through an ethical lens, such as the Fair Priority Model, forces us to confront our moral wrongdoings. Ethical models also provide a foundation for understanding societal values like equity and justice during these extraordinarily troubling times. However devastating this pandemic has been, it has given us the unique opportunity to exercise international collaboration and social justice on an unprecedented global scale. But whether we take this opportunity to do right by society’s most vulnerable members is another question.