Bioethics
The Markkula Center for Applied Ethics explores ethical issues in biology.
What is Bioethics?
by Margaret McLean, senior scholar of the Markkula Center for Applied Ethics
Bioethics involves a reflective, careful examination of issues that arise in biology and medicine, such as end-of-life decision making, DIY biology, biohacking, genetic testing, and the new possibilities of gene editing. It spans a large range of activities that may occur in garages or in laboratories.
Students' Perspectives on Ethical Issues in Health Care

Saving someone’s life could be as simple as pushing a button in the event of an opioid overdose, yet this is information not many know about and even fewer act on. Carrying naloxone is not just a public health initiative, but a moral responsibility all of us carry under the ethical framework of the common good.

Since 2015, there have been 20,000 children who have been sent to wilderness programs in Utah for mental health and behavioral issues. The Troubled Teen Industry and these types of programs are marketed as “rehabilitation” when they are often masking coercion, abuse, and neglect. When adolescent autonomy is neglected and parental consent creates a loophole of harm, is this really treatment or a systemic ethical failure?

Inadequate regulation of anthropogenic nanomaterials—man-made pollutants ranging from 1-100 nm—may reinforce health inequities due to fenceline communities’ heightened exposure.
Police are routinely dispatched to mental health crises, yet these encounters disproportionately result in harm for individuals of color, a pattern long highlighted by racial justice movements like Black Lives Matter. This predictable pattern exposes a deeper ethical tension: can a system grounded in enforcement defend a model that endangers those it is meant to protect?
Fellowships and Internships for Students
Connect with the Ethics Center for student opportunities in our Health Care Ethics Internship, Honzel Fellowship, or Post-Graduation Fellowship in Health Equity and Innovation.

2025 Health Care Ethics Symposium
Symposium with presentations by the 2024-25 Health Care Ethics Interns and the 2024-25 Honzel Fellow from the Markkula Center for Applied Ethics at Santa Clara University.
Access 2025 Health Care Ethics Symposium Recording on YouTube
Commentary on Bioethics

Building an ethical business from day one can be a strategic advantage that attracts partners, talent and investors who care about long-term impact.

Pharmacy closures are a public health emergency in slow motion.

We know that ethics is not just a moral imperative. It is a business strategy.
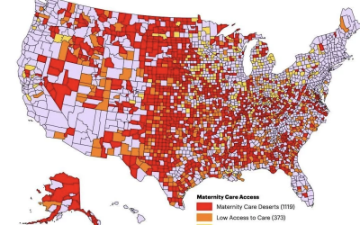
Despite the invaluable contribution of medical advancement to reducing maternal and fetal mortality rates, we must acknowledge the extent to which natural birthing and recovery capabilities are being undermined by efficiency-based health care practices.
Bioethics Materials

Browse curated bioethics pieces on subjects such as end-of-life care, clinical ethics, pandemics, and culturally competent care.

Dive deep into real-life examples of vulnerable patient populations, organ transplantation, and other topics in bioethics.

Hear what our staff and fellows are saying about neurotechnology, current events, and more.

Explore the in-depth guides our staff have organized to model Catholic health care policies, MRSA risk assessment ethics, and beyond.

Health Disparities and COVID - 19
Since the beginning of the COVID-19 pandemic, the African American community and other marginalized groups have been disproportionately impacted by the negative effects of the pandemic in a number of ways. View 2020-21 Hackworth Fellow Amanda Liddell's project on the subject below.
Media Commentary

Guadalupe Hayes-Mota, director, bioethics, quoted by KQED.

Guadalupe Hayes-Mota published in Forbes.

Margaret McLean, Ethics Center senior fellow, quoted by CBS News.

Guadalupe Hayes-Mota, director, bioethics, featured in Santa Clara Magazine.
Culturally Competent Care
Many patients from non-majority ethnicities and/or cultures frequently experience misunderstanding, mistreatment, or marginalization in clinical health care settings. See our compiled resources for health care that is sensitive to the differing values and needs of cultural groups within our diverse society.


End-of-Life Care with Alzheimer’s Disease
What ethical issues arise when terminal neurological diseases, such as Alzheimer's prevent individuals from making medical decisions? This material explores answers to such questions and ethical considerations for end-of-life care with Alzheimer's Disease.